The Epicenters of the Opioid Crisis and What We Can Learn from Them
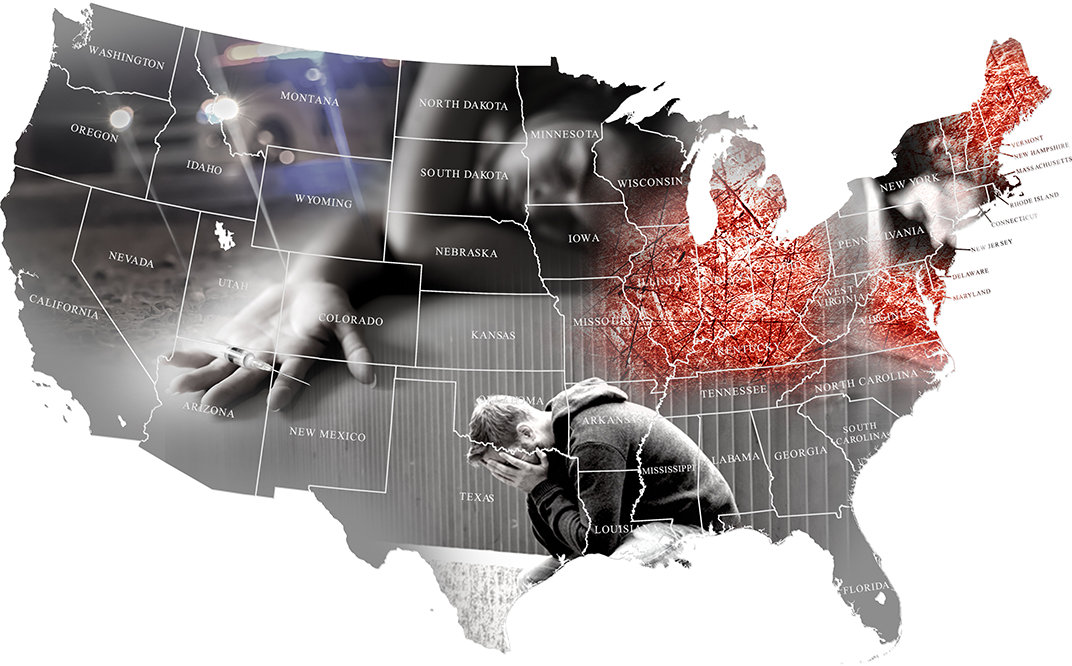
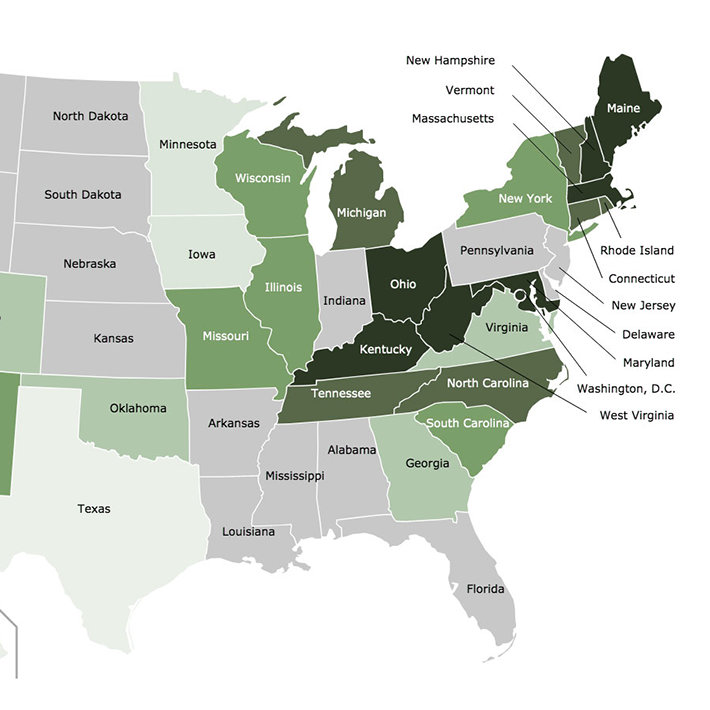
In my morning reading, I happened across an article in U.S. News which discussed the disparity of the opioid crisis in America. The report, written by Robert Preidt, a HealthDay reporter, focused on the opioid turmoil as it has touched down in Indiana, Kentucky, Massachusetts, Maryland, Maine, New Hampshire, and Ohio.
Most of the time when we consider the opioid crisis we discuss the issue on a national level. We attempt innovation of miraculous solutions which will “cure” our problem on a national scale. Some of them have some efficacy, and some don’t.
But I’d like to propose that the real key to tackling and winning against a drug problem lies in figuring out how to solve the problem on a more local level and then applying those successful actions in other locales as well. That’s why I’d like to take a look at some of the hardest-hit areas for opioid addiction and look at what people/governments in those areas are doing to overcome their localized crisis. We’ll take just a brief glimpse at three of the states hit hardest by the opioid crisis, and we’ll discuss what those states are doing to combat the problem.

Ohio
According to the Centers for Disease Control and Prevention’s 2017 reports, Ohio had the second highest rates of overdose deaths, second only to West Virginia. In 2017, 46.3 people died from drug overdoses for every 100,000 residents.
While some strategies have been slow to take effect, the Buckeye State has drafted plans for curbing this death toll. Some of their efforts include cracking down on drug trafficking—a legitimate crime. Ohio lawmakers increased penalties for people caught selling fentanyl, the leading drug killer in Ohio.
Ohio officials also worked to make naloxone more available to both emergency responders and the public alike. Naloxone is a lifesaving overdose reversal medicine. This drug, if applied correctly and expediently, can save a person from the brink of an overdose death. Ohioans now set the bar for community members, families, teachers, emergency responders, and many others who are committed to carrying naloxone with them.
Ohio is also working on expanding addiction treatment for resident addicts. They are increasing treatment options in seven more counties and providing education/training in hospitals to teach staff how to direct overdose patients to treatment centers. Individual hospitals are now doing this. Communities are supporting the treatment centers themselves. Change in Ohio won’t happen overnight. But it is happening now thanks to the state’s increased efforts in this area.

Kentucky
According to the same CDC report, Kentucky has the fifth highest rate of overdose deaths per capita in the country. The state loses 37.2 people to overdoses every year for every 100,000 residents. In light of that, the state has stepped up their efforts considerably in curbing the death toll.
Kentucky made waves when it became the first state to require the use of the state’s Prescription Drug Monitoring Program, or PDMP. PDMP is essentially a program which enables medical practitioners and pharmacies to access a client database. The database contains information on all patients, including where those patients have gotten prescriptions in the past.
PDMPs are invaluable for curbing “doctor shopping” (patient-addicts going from doctor-to-doctor to get prescriptions). The PDMP gives doctors access to any patient’s pharmaceutical history. If a doctor sees (by the patient’s doctor history and prescription history) that the patient in front of them is really an addict seeking pills, the doctor can route the patient to an addiction treatment center instead of issuing yet another prescription.
On a national level, the only catch is that for PDMPs to work, doctors and pharmacies have to use them. Currently, all states have PDMP programs. But their use is not mandatory. It’s voluntary. Kentucky set a precedent by becoming the first state to require physicians and pharmacists to use the program, thus making a bold attack on doctor shopping and prescription drug diversion in the state.

Massachusetts
According to the National Institute on Drug Abuse, Massachusetts ranks in the top ten states for opioid drug overdose deaths as of February 2018. In 2016, there were 1,821 opioid-related deaths in Massachusetts. That’s 29.7 deaths per 100,000 persons. The national average is 13.3 deaths per 100,000 persons. The rate for Massachusetts is more than double the national average.
Synthetic opioids are the biggest cause. In 2012, the state lost 67 people to overdoses on synthetic opioids. But in 2016, the state lost 1,550 people to overdoses on synthetic opioids.
By July of 2018, Massachusetts had had enough, and due to sheer public outcry at the death toll, the House of Representatives was ready to pass a bill which would take decisive action to curb the death toll. The main highlights of the law included making naloxone more available, changing the policy on how pharmaceutical prescribing was done, and piloting medication programs for inmates. We can debate on the efficacy and sense of bringing medications into prisons, but for the most part, Massachusetts was making decisive actions to curb overdoses and addictions.
Further Reading on Taking Action
It’s heartening to catch even a glimpse of what these states are doing to resolve their own substance abuse crises. And it gives us hope, inspiration, and ideas for what we might do in our own communities to follow suit.
Narconon offers a full online library of data on drug addiction and alcoholism, on getting clean, on helpful advice for learning about drug habits and how to help family members, and so on.
In this article, we discussed the implications of opioid addiction issues in key geographic areas. Such an exploration opens the door to further discussion on how to combat the opioid crisis in your area. When we see how opioid addiction is hurting certain areas and what people in those areas are doing about it, it gives us ideas for our own communities, too. But if you want to learn more about opioid drug addiction in general, what it looks like, how it affects people, and how to get help for it, check out this article here.
If you are seeking help for a family member or loved one, you need to learn more about their drug problem, and you also need to know about how to help them. There is much to know on these subjects. Deep down inside, addicts do want help, but their substance abuse habit clouds them, and they cannot find their own way out of it. For more information on how you can help convince your addicted loved one to get help, take a look at this article here.
And if you suspect, but aren’t sure, that a family member or loved one is struggling with a drug habit, check out this article here, which discusses the signs and symptoms of drug use.
Sources:
- https://www.usnews.com/news/health-news/articles/opioid-overdose-deaths-quadruple-centered-in-8-states
- https://www.cdc.gov/drugoverdose/data/statedeaths.html
- https://www.washingtontimes.com/news/ohio-aims-to-curb-overdose-deaths-through-varied-s/
- https://www.pdmpassist.org/pdf/Resources/Briefing_on_mandates_3rd_revision_A.pdf
- https://www.drugabuse.gov/drugs-abuse/opioids/opioid-summaries-by-state/massachusetts-opioid-summary
- https://www.wbur.org/commonhealth/opioid-bill-massachusetts-house
Reviewed by Claire Pinelli, ICAADC, CCS, LADC, RAS, MCAP